Your mouth is not a separate system. It is a gateway. Most adults treat oral care as a cosmetic routine, something to maintain a clean smile and fresh breath, but the biology tells a very different story. Gum disease, tooth decay, and chronic oral inflammation are directly tied to heart disease, diabetes, stroke, and even cognitive decline. Nearly half of U.S. adults over 30 have some form of gum disease right now, many without knowing it. This guide breaks down exactly why your oral health is one of the most powerful levers you have for protecting your whole body.
Table of Contents
- The real risks: How poor oral health impacts your body
- The science: How oral disease spreads beyond your mouth
- Who’s at risk? Oral health and adult wellness after 30
- Prevention and intervention: What works best for your oral-systemic health
- Nuances and expert perspectives: What science knows and what’s still debated
- A smarter step: Support your oral wellness journey
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Oral health is systemic | Your mouth health affects cardiovascular, metabolic, and brain health—it’s not just about teeth. |
| Gum disease is common and risky | Nearly half of adults over 30 have gum disease, increasing risks for chronic illnesses. |
| Evidence supports prevention | Proven oral hygiene and dental care can lower inflammation and improve overall wellness, especially for adults 30+. |
| Innovative aids help—complement, not replace | Smart gum choices support oral routines but don’t substitute for brushing and professional care. |
| Integrated care matters | Dentists and physicians working together provide the strongest defense against oral and systemic disease. |
The real risks: How poor oral health impacts your body
The numbers are hard to ignore. Nearly half of U.S. adults age 30 and older have some form of gum disease, and that figure climbs steeply with age. This is not a minor inconvenience. Gum disease, clinically called periodontitis (a chronic bacterial infection of the tissues supporting your teeth), is one of the most common inflammatory conditions in the world.
What makes it especially serious is the company it keeps. Poor oral health is linked to more than 50 systemic conditions, including heart disease, diabetes, stroke, Alzheimer’s disease, and respiratory infections. These are not loose correlations. They are patterns backed by decades of clinical data showing that what happens in your mouth does not stay in your mouth.
“The mouth is a mirror of the body. Oral disease rarely travels alone.”
Here is a snapshot of the most significant systemic connections:
| Systemic condition | Oral health link | Associated risk increase |
|---|---|---|
| Cardiovascular disease | Gum bacteria trigger arterial inflammation | Up to 2x higher risk |
| Type 2 diabetes | Bidirectional: each worsens the other | 3x harder to control blood sugar |
| Stroke | Oral bacteria found in arterial plaques | Significantly elevated risk |
| Alzheimer’s disease | P. gingivalis detected in brain tissue | Strong emerging association |
| Respiratory infections | Oral bacteria aspirated into lungs | Higher pneumonia incidence |
For anyone focused on enhancing gum health as part of a broader wellness strategy, understanding these connections is the starting point. The mouth is not isolated. It is integrated.
The science: How oral disease spreads beyond your mouth
So how does a bacterial infection in your gums end up affecting your heart or your brain? The mechanism is more direct than most people realize.

When gum tissue is inflamed and bleeding, it creates an open pathway into your bloodstream. Bacteria like Porphyromonas gingivalis slip through that barrier and circulate systemically. Your immune system responds by releasing inflammatory proteins called cytokines, including TNF-alpha, IL-6, and C-reactive protein (CRP). Plaque bacteria trigger immune responses that elevate these markers, raising risk for atherosclerosis (hardening of the arteries) and a cascade of other conditions.
There are two main pathways through which this damage occurs:
| Pathway | Mechanism | Example outcome |
|---|---|---|
| Direct | Bacteria enter bloodstream and colonize distant tissue | Oral bacteria found in heart valves |
| Indirect | Immune response raises systemic inflammation | Elevated CRP damages blood vessels |
Key inflammatory markers involved in this process include:
- TNF-alpha: A cytokine that promotes systemic inflammation and insulin resistance
- IL-6: Drives liver production of CRP and accelerates arterial damage
- CRP (C-reactive protein): A primary marker of cardiovascular risk
- IL-1beta: Amplifies local gum tissue destruction and systemic immune activation
Understanding gum’s role in defense against this inflammatory cascade is part of why functional oral care products are gaining serious attention in the wellness space. The oral health and chronic conditions research published in 2026 reinforces just how central this pathway is.
Pro Tip: Bleeding gums during brushing are not normal. They are a signal that your immune system is already fighting an active infection. Do not ignore it.
Understanding these mechanisms helps us see why your oral hygiene routines are not just about a clean mouth. They are about protecting your whole body.
Who’s at risk? Oral health and adult wellness after 30
Age is the single biggest risk amplifier for oral disease. The data is stark: 68.97% of adults aged 60 and older have periodontal disease, and severe cases double the risk of reduced physical mobility. But the trajectory starts well before 60. By your mid-30s, cumulative bacterial exposure, hormonal shifts, and lifestyle factors begin compounding.
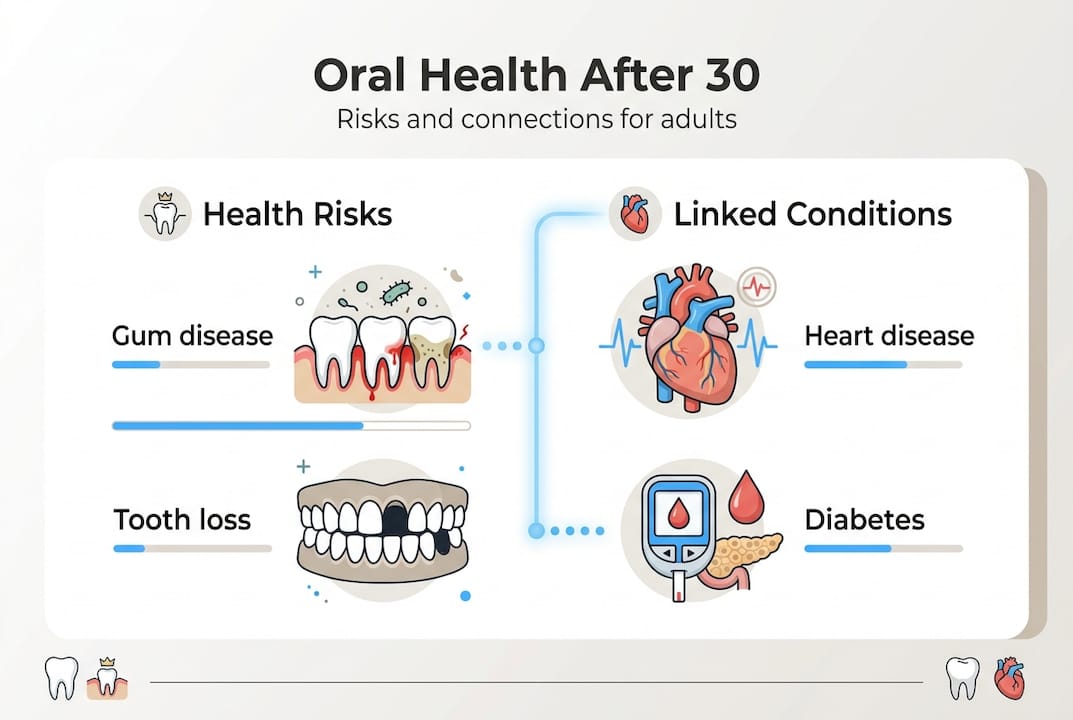
Tooth loss, which is a direct outcome of untreated gum disease, creates a secondary wave of problems. It limits the ability to chew nutrient-dense foods, which increases cardiometabolic risk and accelerates nutritional deficiencies. The mouth is literally the entry point for your nutrition, and when it fails, everything downstream is affected.
The groups most vulnerable after 30 include:
- Smokers and tobacco users: Tobacco suppresses immune response in gum tissue, masking bleeding while accelerating bone loss
- Adults with type 2 diabetes: The bidirectional relationship means uncontrolled blood sugar worsens gum disease and vice versa
- Individuals with chronic stress: Elevated cortisol suppresses immune function, allowing oral bacteria to proliferate faster
- Those with dry mouth (xerostomia): Saliva is your mouth’s natural defense system; reduced flow removes that protection
- Adults on multiple medications: Many common drugs reduce salivary flow as a side effect
For a deeper look at oral health tactics for adults in this age group, the evidence consistently points to early intervention as the highest-return strategy. Waiting until pain appears means the disease has already progressed significantly. More detail on the full spectrum of periodontal disease explained is available through Hopkins Medicine for those who want clinical depth.
Pro Tip: If you have not had a periodontal screening (a simple probe measurement of gum pocket depth) in the last 12 months, request one at your next dental visit. It takes minutes and can catch disease years before symptoms appear.
Now that you know why adults 30 and older face more significant risks, let’s examine what you can do today to improve your oral and whole-body health.
Prevention and intervention: What works best for your oral-systemic health
The good news is that gum disease is largely preventable, and even existing disease responds well to treatment. The evidence base here is strong and growing.
Daily mechanical hygiene is the foundation. Brushing twice daily with fluoride toothpaste, flossing once daily, and avoiding tobacco removes the bacterial biofilm (plaque) before it mineralizes into tartar. No supplement or product replaces this. But professional care adds a layer that home routines simply cannot match. Dental cleanings remove calcified tartar from below the gumline, where brushes and floss cannot reach.
The systemic payoff of treating gum disease is measurable. Periodontal treatment reduces systemic inflammation, lowers HbA1c (a three-month average blood sugar marker) in diabetic patients, and drops TNF-alpha and CRP levels. That is not just better gum health. That is better metabolic health.
“Treating the mouth is treating the body. The two are not separate clinical territories.”
Top habits and interventions for adults 30 and older:
- Brush for two full minutes, twice daily, using a soft-bristle brush
- Floss daily, or use an interdental brush if flossing is difficult
- Use an antimicrobial or fluoride mouth rinse as an adjunct, not a replacement
- Schedule professional cleanings every six months, or every three to four months if you have active gum disease
- Quit tobacco in any form
- Manage blood sugar if diabetic, as glycemic control directly improves gum tissue response
- Consider gum chemistry and dental health innovations that support remineralization and salivary flow between meals
For a clinical overview of what prioritizing gum health looks like in practice, Cleveland Clinic provides a solid framework.
Nuances and expert perspectives: What science knows and what’s still debated
Here is where intellectual honesty matters. The associations between oral disease and systemic conditions are robust and consistent across populations. But strong associations exist without full causation being proven for every link. Many of these conditions share underlying risk factors, particularly chronic inflammation, poor diet, smoking, and socioeconomic stress.
This does not weaken the case for oral care. It actually strengthens it. If inflammation is the shared driver, then reducing oral inflammation is one of the most accessible ways to lower your overall inflammatory burden. You do not need to wait for a definitive causal trial to act on that logic.
Experts increasingly call for integrated care models where dental providers and medical providers collaborate, especially for patients managing diabetes or cardiovascular disease. Oral health screening in cardiology and endocrinology clinics is gaining traction as a prevention tool.
Risk factors worth knowing:
Modifiable (you can change these):
- Tobacco use
- Poor diet high in fermentable sugars
- Inadequate oral hygiene
- Uncontrolled blood sugar
- Chronic stress
Non-modifiable (you manage around these):
- Age
- Genetic predisposition to inflammatory response
- Certain autoimmune conditions
For tips for oral care routines that address the modifiable side of this equation, the focus should always be on consistency over perfection. And for a broader view of integrated oral health care, Guardian Life’s research hub is worth bookmarking.
A smarter step: Support your oral wellness journey
You now understand that oral health is systemic health. The bacteria, the inflammation, the pH chemistry in your mouth all have downstream effects that reach your heart, your brain, and your metabolic function. The foundation is always mechanical hygiene and professional care. But what you do between brushing sessions matters too.
Scandigum is built on exactly this principle. Rather than a flavor-forward product, it is a bio-optimization delivery system designed to work with your mouth’s own chemistry. By stimulating salivary flow, supporting remineralization, and leveraging buccal absorption, Scandi Gum premium gum fits into the gaps in your oral care routine where conventional products stop. If you want to understand the full science behind how it works, the dental chemistry explained breakdown covers the remineralization mechanism in detail. This is not a replacement for your dentist. It is a smarter way to support your biology every day.
Frequently asked questions
Can poor oral health really affect heart disease risk?
Yes. Gum disease is linked to heart disease through bacterial spread and elevated inflammation markers, though researchers note that direct causation is still being studied across long-term trials.
Does chewing gum actually help your oral health?
Sugar-free gum with xylitol can reduce cavity risk by stimulating saliva and neutralizing acids, but mechanical removal and antimicrobials remain the primary tools for managing gum disease.
How does periodontitis treatment improve whole-body health?
Treatment lowers HbA1c and inflammation, which directly improves outcomes for diabetic patients and reduces systemic inflammatory markers linked to cardiovascular risk.
Is the oral-systemic health link proven for everyone?
Strong associations exist across populations, but causality is not fully established for every condition. The practical takeaway is to focus on modifiable risks like hygiene, diet, and tobacco use regardless of where the science lands on causation.
